Dr. Heather Ross, TRANSFORM HF co-lead and Head, Division of Cardiology UHN-SHS, led a team on a trip to Moosonee and Moose Factory in May 2022 to continue to deepen our partnership with Weeneebayko Area Health Authority (WAHA).
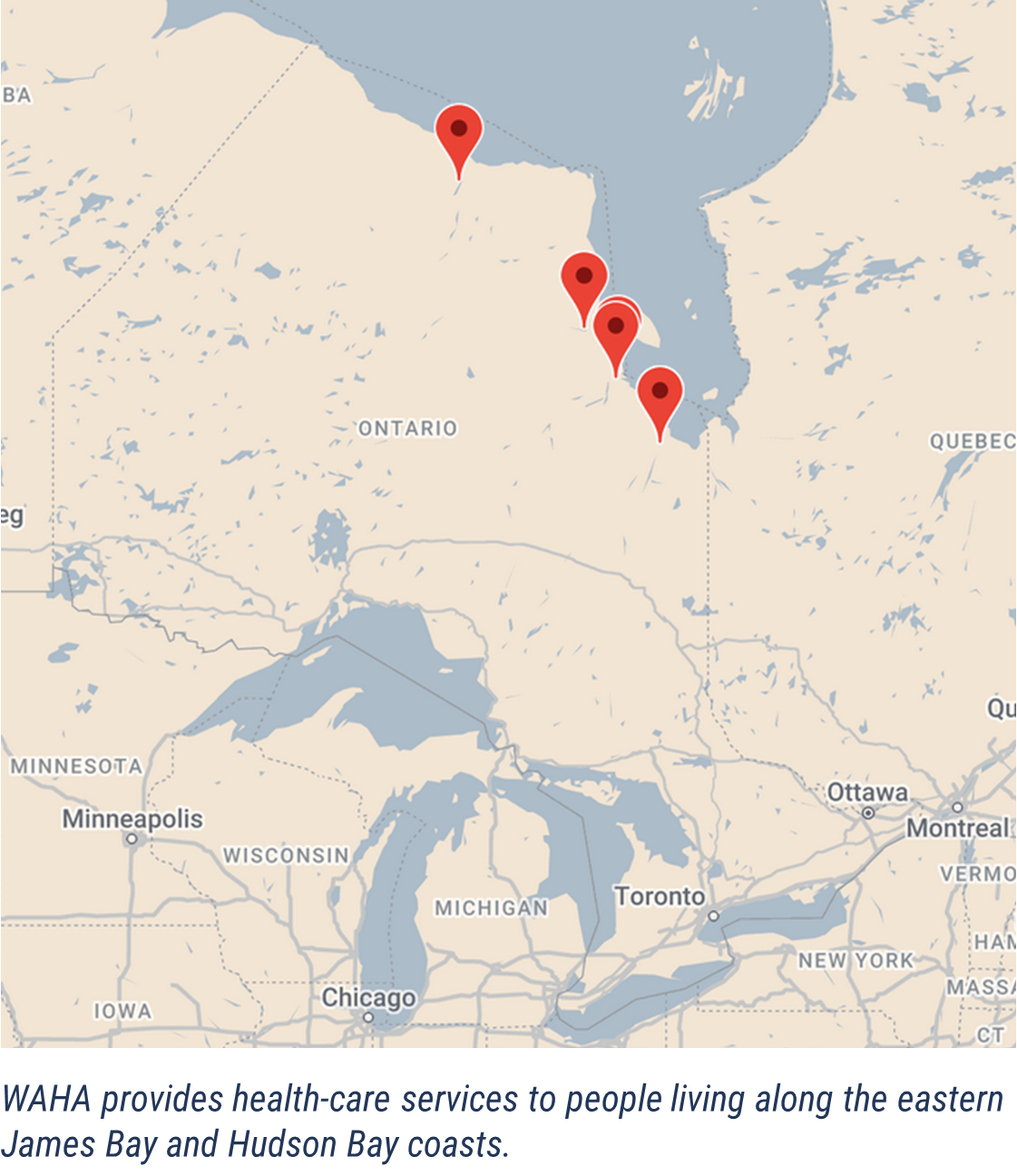
WAHA is a regional, community-focused organization dedicated to providing holistic health care reflective of the distinct needs of peoples living along the Northeastern Ontario James and Hudson Bay coasts – as close to home as possible.
“We are thrilled to partner with an organization like UHN who shares a mutual interest in community-led health care, which helps us to reinforce our mission of providing optimal care close to home,” says Lynne Innes, President and Chief Executive Officer, WAHA.
Following a COVID-imposed hiatus, the collaboration to address heart failure in the Weeneebayko region was renewed with a visit consisting of in-person clinics, community outreach, and a sharing circle.

Cardiovascular disease: A priority for WAHA communities
Indigenous populations across Canada experience a higher burden of cardiovascular disease (CVD) morbidity and mortality compared to the general populationi, with a rapid increase in cardiac risk factors leading to heart failure.
Historical oppression, racism, and the undermining of traditional lifestyles contribute to impaired diet, low trust in the health care system, barriers to access to education and health literacy, and other disparities in social determinants of healthi,ii. A recent study by Vervoort et al. linked these contributing factors to delays in seeking, reaching, and receiving care, and ultimately to impacted cardiovascular health and worse long-term outcomes among several First Nations communities across Canadaii.
Many First Nations communities in the James and Hudson Bay region are remote with limited access to specialized cardiac care, with similar CVD outcomes. According to a report by the Mamow Ahyamowen partnership: “Our community members were more likely to have a history of heart failure than Ontario overall in every age group where heart failure occurred in our communities.” Heart failure mortalities in these communities continue to climb, increasing by just under 10% between 1992 and 2014iii.
Community-based Partnership
After an initial outreach in 2017 as part of a research proposal development, the partnership deepened with a first visit in 2019. “Our partnership has always been centered on ensuring people in the James and Hudson Bay region have access to the care they deserve,” says Dr. Ross.
The partnership comprises clinical care and research, and will hopefully expand to education.
- Working with local physicians and clinics, WAHA patients are referred to UHN’s Heart Function program to access specialist care, including virtual, in-person, and remote management by Medly.
- WAHA and UHN are collaborating on a community-based research project to understand what heart health means for people in the region, and to reimagine and co-create models of digital health that respond to the region’s unique needs, strengths, and context.
With referrals from WAHA physicians, clinics were held at both the Moosonee Health Clinic and the Weeneebayko General Hospital in Moose Factory. Working with WAHA’s executive team and local Chiefs and Councils, the team aims to travel to all coastal First Nation communities to provide heart failure care on an ongoing schedule (i.e., Peawanuck, Fort Albany, Attawapiskat, and Kashechewan).
WAHA also strives to inspire the next generation of health care providers through mentoring. The UHN/TRANSFORM HF team joined in the effort, highlighting STEM opportunities at UHN and University of Toronto and pathways to medical school for high school students at Northern Lights Secondary School in Moosonee and Delores D. Echum Composite School in Moose Factory.
Elder Greg Spence led a sharing circle focused on heart health in Moosonee during the team’s visit. Local community members shared their stories and perspectives on heart health, as well as identified current challenges faced when accessing care and potential solutions. This is the first of what is hoped to be sharing circles in each of the six communities. The sharing circle also explored the implementation of a digital health self-management program for heart failure in the WAHA region. “Right now, community members who require treatment for heart failure must travel 850km by air, bus, or train to Kingston General Hospital,” explains Dr. Ross. “Digital tools may allow patients access to high-quality, preventative care right in their community – but devices and models of care need to be developed in collaboration with community members, from ideation to implementation.”

Dr. Ross is planning another trip with WAHA’s leaders in the fall that will add Peawanuck on Hudson Bay to the itinerary. Eventually, it is hoped that all six communities will be engaged in an ongoing schedule of commitments to deepen the connections and provide meaningful care. As the partnership continues to grow, Dr. Ross hopes it may facilitate the co-creation and testing of digital health devices grounded in cultural safety and respect for Indigenous ways of knowing and being, in collaboration with TRANSFORM HF’s network and community members.




